Medically reviewed by Mary Jane Minkin, M.D.
If you’re looking for a safe, effective and hassle-free way to prevent pregnancy, long-acting reversible contraception (LARC) may be a good option for you.
We reached out to Mary Jane Minkin, M.D., a clinical professor of obstetrics, gynecology and reproductive sciences at the Yale University School of Medicine and a member of HealthyWomen’s Women’s Health Advisory Council, to find out what questions you should ask your healthcare provider (HCP) if you’re considering using LARC.
What is long-acting reversible contraception (LARC)?
As the name suggests, long-acting reversible contraception is effective birth control that lasts a long time and can be easily reversed.
Most oral contraceptives would be close to 100% effective if we weren’t human, and we could remember to take things at exactly the same time every day and never forget anything. But unfortunately, with real-world usage the numbers are more like 91% or 92%.
That’s where the concept of long-acting reversible contraception comes in. It takes out the possibility of human error.
What are the different types of LARC?
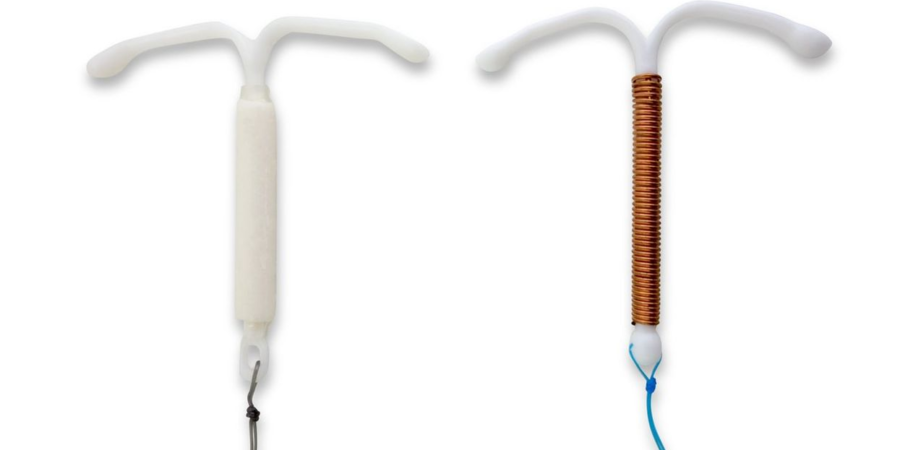
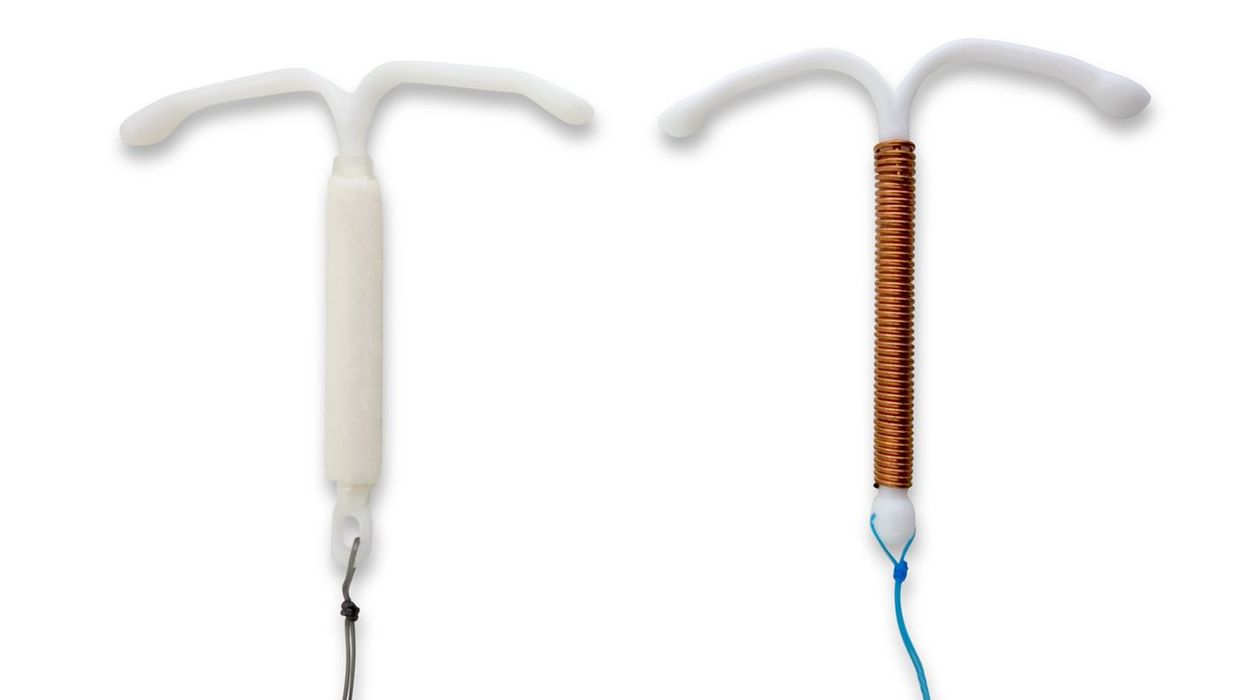
The intrauterine device (IUD) was one of the first LARC methods. IUDs are small devices that are inserted into the uterus. They are approved to last anywhere from 3 to 10 years, depending on the brand. Hormonal IUDs, such as Mirena, Skyla, Liletta and Kyleena, contain progestin, a man-made version of the hormone progesterone. ParaGard, which is made of copper, is currently the only hormone-free form of LARC.
Many women like hormonal IUDs because they can help control bleeding, meaning you may not get a period, or your periods will be very light. And you can become fertile fairly quickly after removing them. A downside is that they can only be put in by a HCP, and insertion and removal can cause some pain.
Then there’s the contraceptive implant, Nexplanon, which is a progestin-releasing rod that’s put in your arm. It lasts for three years. The implant is a good option for people who want long-lasting hormonal birth control but want to avoid estrogen. The most common concern people have about the implant is that a lot of people get breakthrough bleeding with it. And it does need to be inserted and removed by an HCP.
How effective are these LARC methods?
They’re very effective at above 99%.
Who can use LARC methods of contraception, and who shouldn’t?
Most women can safely use LARC methods, although all forms of hormonal birth control have some circumstances where they shouldn’t be used. For example, women who have unexplained bleeding should avoid LARCs until they can figure out what’s causing them to bleed. A HCP can offer specific guidance around safety concerns.
It’s also important to note that LARCs don’t protect against sexually transmitted infections (STIs). Condoms are the only form of birth control that also prevents STIs.
What are some common misconceptions about LARC methods?
I think the biggest misconception about LARC is that these methods can negatively affect a woman’s fertility in the long term. And that’s not the case. By definition, LARC is reversible.
Another misconception is that you have to keep them in the entire time they’re active, but that’s not true. You can remove LARC at any time.
What questions should women ask themselves in order to make an informed decision about birth control? What factors do you consider when making recommendations?
Whether a woman is starting birth control for the first time or contemplating a switch after many years with the same form, I always want to help guide her toward whichever one will make her happy — the one that will best meet her individual needs.
Is she only looking to prevent pregnancy, or does she want to control bleeding too? Does she want to start a family sooner rather than later? Other factors to consider include ease and efficacy.
With so many safe and effective options available, women can choose the one that best meets their unique needs.
This resource was created with support from Organon and Co. and Sebela Women’s Health, Inc.